THE RADIOTHERAPY TEAM
As a patient, friend or family member you are likely to encounter different team members while visiting a radiation-oncology department. Below is an overview of individuals and organisations one might be in contact with. They are not necessarily represented in the order you might see them, and not all persons or functions exist in all departments.
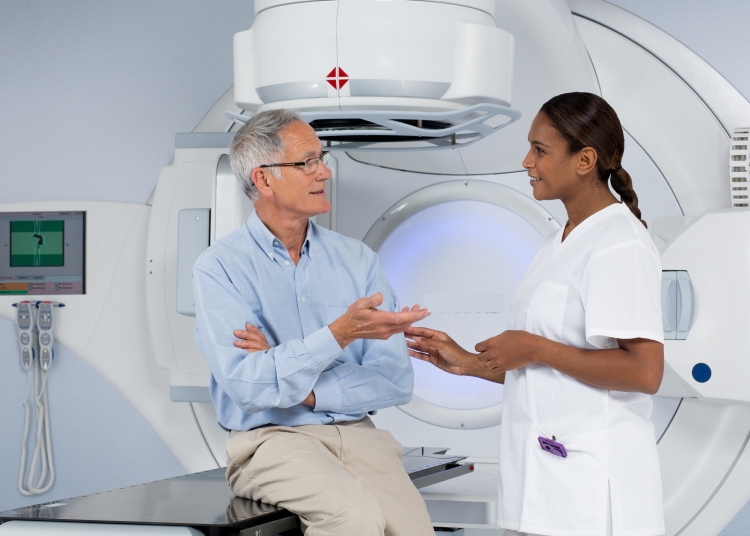
At the level of the radiotherapy department
- The radiation oncologist
- The radiation technologist at the simulator
- The radiation technologist at the treatment machine
- The volunteers
- The secretarial staff
- The medical physicist
- The dosimetrist
- The psychologist
- The dietician
- The social support team
- The nurses
- The support staff
- The technicians from the department
- The technicians from the companies providing the radiotherapy machinery
- The quality manager
The radiation-oncologist
The radiation oncologist is a medical specialist. The specialty of radiation-oncology requires an additional 5 years of training after having obtained the basic diploma of medicine.
The radiation technologist at the simulator
The simulator is the scan used to prepare the treatment. It is operated by technologists with a degree in nursing or medical imaging techniques.
The radiation technologist at the treatment machine
The treatment machine is manned by 2 to 4 technologists, usually with a degree in nursing, but staff members with other backgrounds or a specific training as radiation technologists are also present. This is the team the patient will be most often in contact with.
Volunteers
To assist patients in spending a comfortable time in the radiotherapy department, sometimes volunteers can be present to help people with mobility problems, to offer a listening ear, to bring drinks, to create a friendly atmosphere in waiting rooms, ...
The secretarial staff
Behind the scene of a radiotherapy department, quite some administration needs to be done. Patients might also see the secretarial staff at the reception desk.
The medical physicist
Quality control and calculating the behaviour of the treatment beams in the human body or the two main tasks of the physicist. In the very advanced technical radiotherapy nowadays offered, physicists play a leading role. Patients will however rarely come in contact with the physicist, though a physicist is always present in the background when a radiation treatment is done.
The dosimetrist
To allow the medical physicist to concentrate on the quality control and on long-term technical developments, the dosimetrists take over the 'treatment planning', which is the calculation of the treatment based on the images obtained during the simulation. Patients will rarely meet the dosimetrist.
The psychologist
All radiotherapy departments offer the possibility to meet or be referred to a psychologist. He or she is part of the 'oncology support team (OST)' offering a wide range of help for patients and family members suffering from the psychological burden and other problems induced by the disease or the treatment. The psychologist can offer specific psychological help, and when required can organize further follow up or referral to other support team members.
The dietician
Most departments offer the possibility to meet a dietician (nutritional counsellor) because the cancer, the systemic and sometimes also the radiotherapy treatment might influence eating patterns, the metabolism of the body or the appetite.
The social support team
While the oncology support team focuses on the patients with his/her illness, the social support team will focus on the patient in his/her relation with the community. This involves helping with obtaining reimbursement, transport, recognition as a disabled person, ... Advise on how to deal with family members, colleagues at work, children, ... is also available.
The nurses
Above the 'radiation technologists' were presented. In some departments, these are not all nurses. Which means that specific tasks which require a nursing degree will be organised by colleagues with such a degree. For instance taking blood samples, evaluating blood tension, taking care of wounds, ... In some departments, nurses assist the radiation oncologists during outpatient consultations, which means that nurses can (re)explain part of the information that was given by the radiation oncologists. Some routine 'preventive' consultations can also be done primarily by nurse practitioners.
The support staff
In larger departments all of the above functions can be assisted by team members without a specific degree, but who can help more trained colleagues wherever required.
The technicians from the department
Some departments have technicians and engineers keeping an eye on the correct technical functioning of the complex radiotherapy machines.
The technicians from the companies providing the radiotherapy machinery
Radiotherapy machines require maintenance and other tasks that can not be done by the technicians from the department. These are done by specialist technicians from the manufacturer of the machine. These service engineers can be foreigners, servicing the machines all over Europe.
The quality manager
Radiotherapy departments have a long tradition in quality control, in the past mainly managed by the physics team. But quality goes way beyond the physics aspects of the treatment, so nowadays a dedicated quality manager is present in all radiotherapy departments.
At the level of the hospital
The medical oncologist
The organ specialist
The specialist in nuclear medicine
The medical imaging specialist (radiology, ...)
The pathologist
The one-day clinic staff
The in-patient department staff (in case of a hospital stay)
Outside the hospital
The general practitioner
The physiotherapist
The staff from your medical insurance
Scientific organisations
Radiation oncologists and all other team members active in a radiotherapy organisation do profit from continuous medical education. National and international organisations offer a platform where this education is organised and where also scientific work is presented. We will not discuss this in detail, but more information can be found on the Who is who in Belgium page in the section for medical professionals.
